

Dental care is an important and expanding area of pet health. Often, after we have performed dentistry, our patients’ parents tell us that they act more energetic and playful than they have in years!! The condition of our furry friends teeth directly impacts on their general wellbeing. Here are some common questions we get asked.
Q: Why must my pet undergo anaesthesia for a teeth scale and polish?
A: The most important part of the cleaning is the removal of plaque and tartar under the gumline. This is just not possible in an awake pet. Polishing is an important final step, which would also be difficult to do, leaving the the teeth surfaces smooth and making it less likely for plaque to adhere. A full anesthesia, as opposed to a sedation, allows us to place a tube in the windpipe, thus preventing infection of the lungs from the numerous bacteria in the plaque being scaled off the teeth.
Q: I am worried about my 13 year old dog undergoing anesthesia for a dental procedure. Is it possible for a dog to be “too old” to benefit from professional dental care?
A: Some people tell us about pets that have had problems or died under anesthesia. Fifteen or twenty years ago many of these concerns would be valid reasons for not proceeding with an elective procedure in an older pet. Fortunately, things have changed for pets having anesthesia today. Contemporary anesthesia is much safer in several ways.
First, pre-anesthetic blood testing helps us to recognize those pets that are having internal problems that aren’t yet recognizable by their owners at home. If a problem is found, we can try to resolve it before allowing the pet to undergo anesthesia.
Second, modern inhalant gas is much safer. And as mentioned above, the tube in the windpipe protects against contamination of the lungs by oral or stomach matter.
Third, monitoring anaesthesias has changed from merely watching to see if the dog is breathing, to using technology for tracking pulse rate and quality, oxygen saturation, respiratory rate, temperature. When pets are being monitored, it allows veterinarians and nurses to detect abnormalities and avoid anaesthetic problems.
Fourth, all pets undergoing dental care receive fluid therapy by intravenous catheter during anaesthesia, to maintain vascular volume and blood pressure. This protects sensitive brain and kidney cells. We also use thermal support to prevent hypothermia during anesthesia which can change the rate at which drugs are processed.
Age is not a disease, and mature pets that are otherwise healthy are able to tolerate anaesthesia well. A pet that is older is more likely to have more severe periodontal disease and thus more pain. These animals still need care in order to maintain the quality of their lives. Taking care of their gums and teeth is also one of the best ways to extend their lifespan.

Q: Why is cleaning my pet’s teeth more expensive than cleaning my teeth? Why is it more expensive than the last time his teeth were cleaned a few years ago?
A: The cost of dental care for pets has certainly increased as the quality of anaesthesia, cleaning, and services have increased. We want to provide safe anaesthesia and a service that actually helps to treat pain and prevent progression of disease and to do that we need specialised equipment. Most of this equipment is not necessary when humans teeth are cleaned because we are not undergoing anaesthesia. Also, remember that usually our human dental hygienist is performing a routine preventative cleaning, before hardly any tartar has built up on our teeth. Pets rarely get dental care this early and thus their cleaning is not a true preventative.
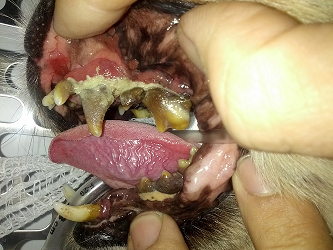
Q: How can periodontal disease hurt my pet?
A: The possible local (ie in the mouth) effects of periodontal disease are pain, infection of the gums, and loss of teeth. Chronic infection of the periodontal tissues allows bacteria to enter the blood resulting in seeding of the internal organs (heart, kidneys, liver) and may lead to serious infections in these organs as well.
Q: The veterinarian has recommended extraction of some of my pet’s teeth but will he still be able to eat without these teeth?
A: Yes. Our goal in veterinary dental care is for our patients to have mouths free of infection and pain. It is much better to have no tooth at all than to have an infected tooth with a root abscess or a painful broken tooth. We have many dog and cat patients that are able to eat a regular diet with few or even no teeth! Sometimes a veterinary dental specialist can offer root canals or more advanced therapy to save teeth. We will offer you a referral if there is a possibility of saving teeth.

Q: I can’t tell that my pet is in any pain even though he has broken teeth and red inflamed gums. Wouldn’t he stop eating if he was in any pain?
A: Some pets will stop eating all together when their teeth, bone, and gums hurt badly enough. The vast majority, however, will find some tactic to keep themselves eating. They may chew on the other side of their mouths or swallow their kibble whole. Pets have an extremely strong instinct to survive no matter what discomfort they feel. Sometimes the symptoms of periodontal disease are so vague that we don’t notice them. Pets may be reluctant to hold their toys in their mouths, be less playful, resent having their teeth brushed, have a hard time sleeping, or, sometimes have no outward symptoms at all.
Q: How often should a routine dental cleaning be performed?
A: Every patient is different so this is a hard question to answer. Usually the smaller dogs should have their teeth cleaned earlier and more often because their teeth are more crowded in their mouths. Bigger dogs may not develop tartar as quickly but their mouths should be monitored closely for any broken teeth. Cats are all individuals and should be examined closely for any excessive gingivitis (inflamed gums) which may be an indication of some special cat diseases.


